Addiction Models in Rats and Mice

Back to Pharmacology and Toxicology Assessment top page
Addiction is characterized by obsessive-compulsive seeking for a substance, and consequently obtaining that substance, with a progressive loss of behavioral control [4]. As such, addicts become consumed with obtaining and using the substance of choice despite negative consequences. For example, more than 3.3 million people worldwide die from complications of alcohol addiction [1]. In 2017, an estimated 48.7 million Americans over the age of 12 were cigarette smokers. In the same year, ~140.6 million Americans in the same age category were alcohol users, of which 66.6 million were considered binge drinkers. Furthermore, 30.5 million are illicit drug users, with most being marijuana users and the remainder abusing cocaine, hallucinogens and prescription drugs [5]. Overall, addiction costs the US an estimated $700 billion per year [2].
There are environmental as well as genetic factors that contribute to a person’s vulnerability to addiction. These factors include adverse early life experiences, exposure to drugs, familial genetics and trauma [6]. Genetic factors constitute almost half of the risk for addiction [7]. Variations in specific genes can make a person more susceptible to becoming addicted to certain substances, and there is ongoing research into how these genes truly contribute to the development of addiction.
Addiction is difficult to study in humans due to safety and ethical concerns as well as the long duration of the addiction process. Preclinical models are, therefore, necessary to develop behavioral and pharmacological treatments for addictive behavior [2]. These models provide timely approaches that incorporate the genetics, anatomy and neuropharmacology of potentially therapeutic compounds in controlled environments [8], and they have predictive validity in that they have translated to the clinic. For example, acamprosate, naltrexone and nalmefene are all medications that were first developed with animal alcohol models, and the actions of these drugs were demonstrated successfully in humans [3].
Conditioned Place Preference (CPP) Method
Induction:
The following is an approach for morphine in rats, but the setup is similar for mice. The apparatus for conditioned place preference (CPP) consists of 3 chambers of identical size. The middle chamber is considered a neutral starting position, while the 2 side chambers have differing floor textures (e.g. smooth vs. mesh grid) and visual cues (e.g. checkered vs. striped wall pattern). All animals will be acclimated to the testing room for 1 hour prior to any test sessions or conditioning sessions. During pre- and post-conditioning test sessions the animal will be started in the middle chamber and allowed free access to all 3 chambers.
The pre-conditioning test (day 0, 15 mins) will determine an animal’s preference baseline. Animals with unconditioned preferences for one context over the other (> 100s) will be excluded from the study.
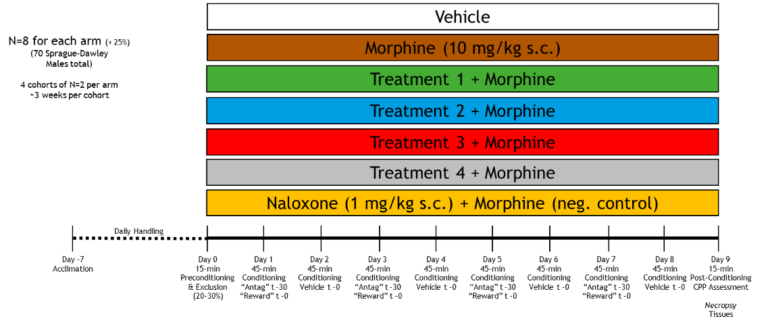
Conditioning will proceed over 8 days of alternating treatments (days 1, 3, 5 and 7) with vehicle control (days 2, 4, 6 and 8). The treatments will include vehicle negative control, morphine positive control (10 mg/kg s.c.), and the other arms will be up to the client. Agents hypothesized to modify the acquisition of morphine CPP will be administered 30 minutes before conditioning, while morphine will be provided immediately before conditioning. Each conditioning session will occur once per day, last for 45 minutes, and the animal will be confined to the same context for both the entire session and for all treatment conditioning days. On vehicle control days, the animal will be paired to vehicle in the alternative context. The animals in each group will be counterbalanced in that 50% of non-excluded animals will have the treatment paired to one context, while the remaining 50% will have the treatment paired to the other context. Such counterbalancing will also occur in the vehicle negative control group.
Disease Parameters & Clinical Assessment:
Post-conditioning preference testing will occur on study day 9. Again, the animals will be started in the middle chamber and allowed free access to all 3 chambers for 15 minutes. The CPP score will then refer to the differences in time spent between the treatment-paired chamber and the vehicle-paired chamber (Zhu et al. 2020). If an animal prefers the compound of interest, it will spend more time in the chamber that is associated with the drug. Conversely, if the animal perceives an adverse effect, it will spend more time in the chamber associated with the vehicle control. It should be noted that CPP can also be used in reverse as conditioned aversion or as a pain assessment procedure. In these cases, an animal will spend more time in the context that is associated with the alleviation of pain or other aversive stimuli.
Sample Study Design:
2-bottle choice method
Induction:
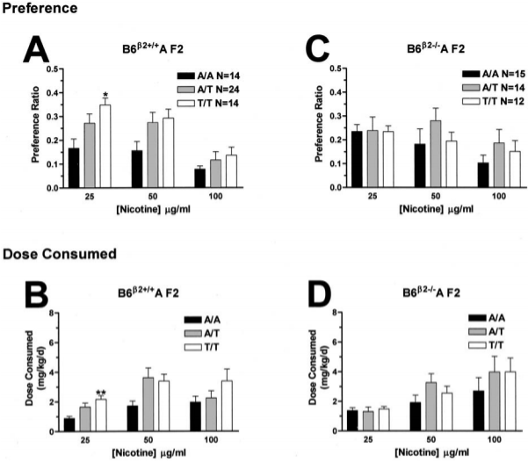
Using a two-bottle choice preference protocol, singly housed animals are given a choice between an aqueous compound in water and water itself. Depending on the compound and potentially adverse effects of taste, a vehicle solution of 0.3% sucrose may be used. Animals begin with a low dose of the compound, the dose will increase every four days, and the highest dose will occur from days 8-12. The positions of the two bottles on the animal cage will be switched daily to reduce side preferences.
Disease Parameters & Clinical Assessment:
Liquid amounts in each bottle will also be recorded daily at the same time as bottle switching to measure the amount of compound consumed in a 24-hour period. The amount of drug consumed at each dose, as well as the preference ratio between drug and vehicle, then serve as a measure of abuse potential.
Other Disease Parameters & Clinical Assessments:
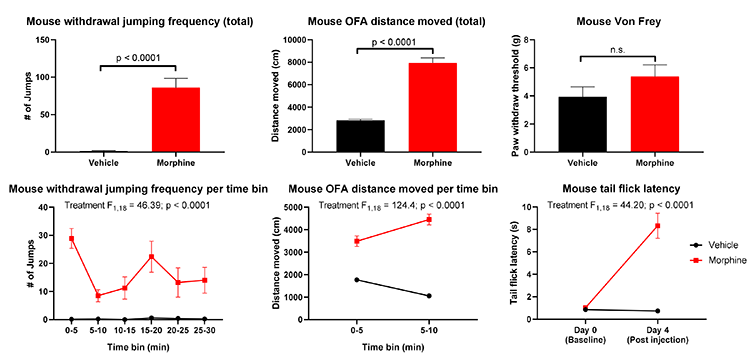
After drug exposure, animals can also be challenged in the following assays-
- Nestlet shredding/nest building: homecage behavior for anxiety and distress
- Light-Dark box (LDB): anhedonia and anxiety
- Open Field arena (OFA): spontaneous locomotor activity and anxiety
- Elevated Plus Maze (EPM): anxiety
- Marble burying: homecage assessment of perseverative and repetitive behaviors
- Hargreaves: measures pain and heat thresholds of the animal
- Von Frey: evaluation of mechanically-induced pain or sensitivity (allodynia)
- Gait analysis: weight-bearing pain
- Morris water maze (MWM): learning, memory and cognitive function
- Contextual (and cued) fear conditioning: learning (aversive stimulus) with context
Related Pages
- Glioblastoma Models in Mice
- Epilepsy Models in Rats and Mice
- Addiction Models in Rats and Mice
- Cognition Models in Rats and Mice
- Experimental Autoimmune Encephalomyelitis (EAE)
- Developmental Milestones Aka Functional Observation Battery
- Anxiety Models in Rats and Mice
- Depression Model in Rat
- Fragile X Syndrome (FXS) in Mice
- Parkinson’s Disease Models in Rats and Mice
- Alzheimer’s Disease Model in Mice