Non-Lethal Caerulein-Induced Pancreatitis (Rat, Mouse)

Induction:
On study day 0, mice or rats are randomized by body weight and intraperitoneal caerulein injections are initiated. Animals receive hourly caerulein injections for up to 9 consecutive hours (time points: 0, 1, 2, 3, 4, 5, 6, 7, and 8 hours). Number of doses determines model intensity.
Disease Parameters:
Caerulein-induced acute pancreatitis in mice is a well-studied model of the disease, which is characteristically a mild, necrotizing, self-limiting, and highly reproducible pancreatitis. The initiation of the disease is thought to be mediated through premature intracellular activation of zymogens in the acinar cells, which leads to activation of a cascade of digestive zymogens that results in acinar cell necrosis and mild pancreatic edema followed by an inflammatory response. Hyperamylasemia caused by leakage of amylase from injured acinar cells is also indicated.1,2
Dosing Paradigms:
- Begin dosing on study day 0 at 1 hour or 30 minutes prior to the first caerulein injection, or at the time of injection, and continue until necropsy 8, 12, or 24 hours after the first caerulein injection.
- Begin dosing X days prior to caerulein injection (day X) and continue until necropsy 8, 12, or 24 hours after the first caerulein injection.
- Route of administration: SC, PO, IP, IV
Clinical Assessment:
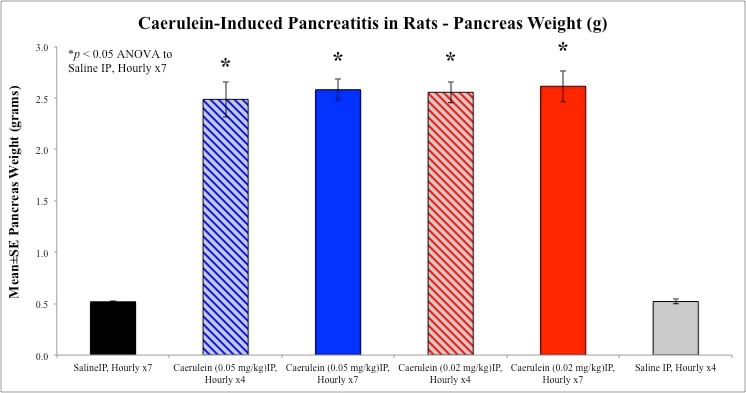
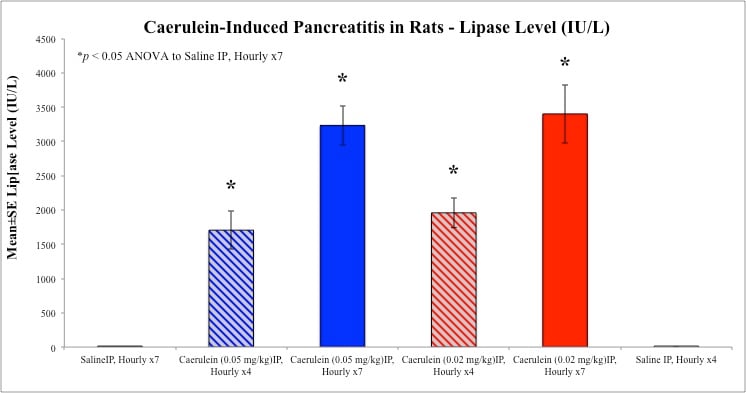
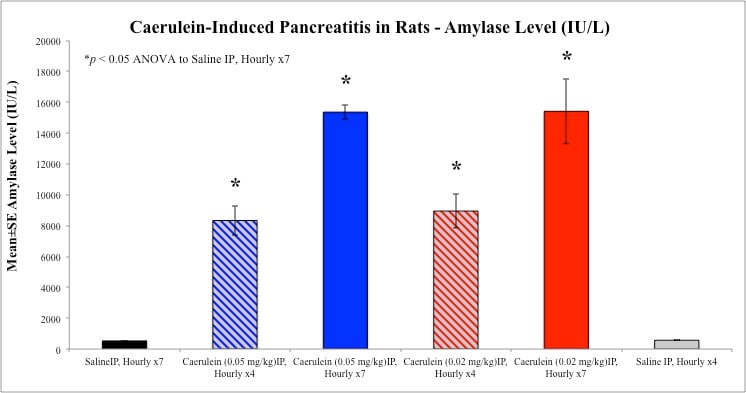
At necropsy, pancreata are removed, trimmed, and weighed. Blood samples are drawn via cardiac puncture from Isoflurane anesthetized animals into serum separator microtainer tubes for clinical chemistries. Samples are analyzed for serum amylase (AMY) and lipase (LIP) levels.
Histopathological Assessment:
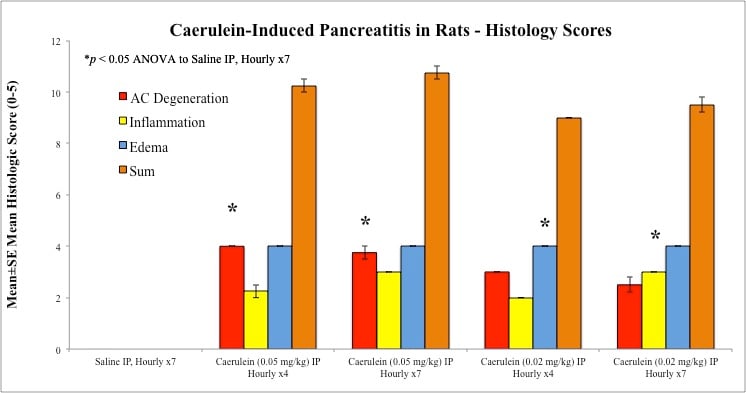
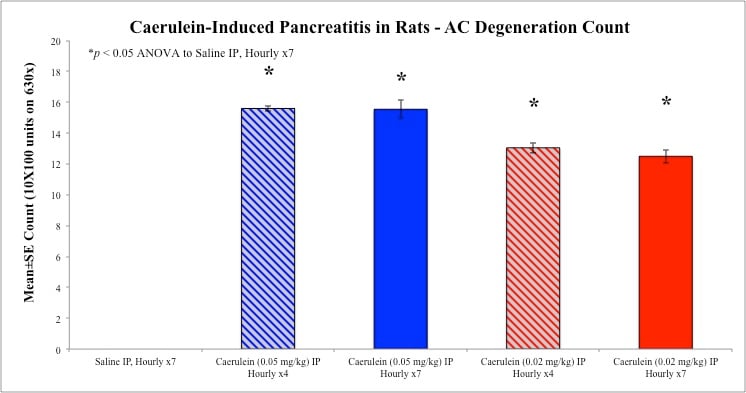
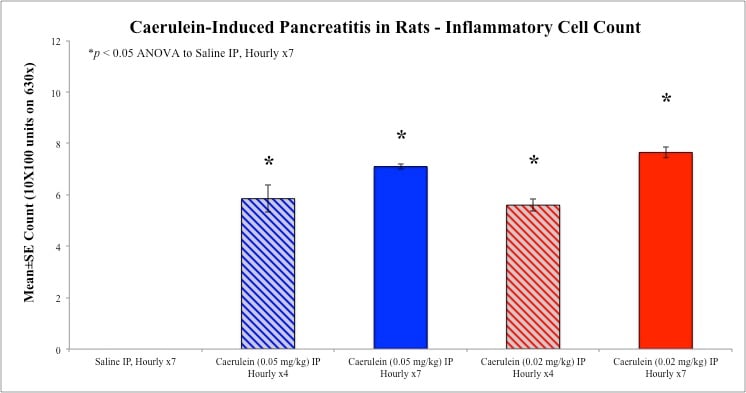
Pancreas sections were examined for degree of necrosis, vacuolization, inflammation, and edema according to these methods.
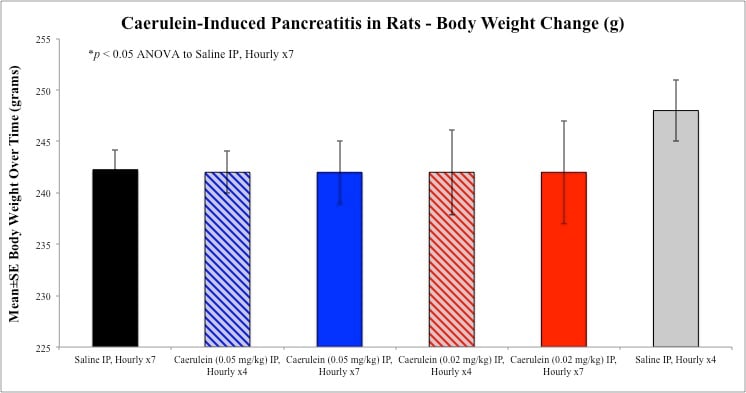
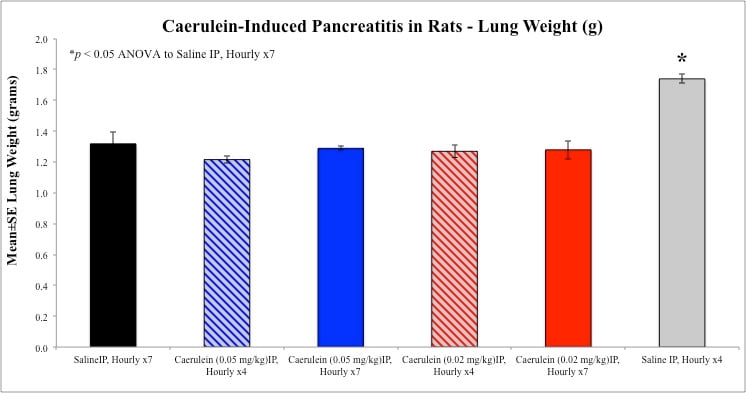
Sample Data (Click on image to enlarge):
Rat
For additional examples of positive controls, please contact us.
Notes:
Pancreatitis is an inflammation of the pancreas that occurs when pancreatic enzymes that digest food are activated in the pancreas instead of the small intestine. It can be acute in nature, beginning suddenly and lasting a few days, or chronic, lasting many years. Several etiologies are known to induce acute pancreatitis, including biliary tract stones, ethanol abuse, trauma, tumors, and idiopathic factors. Clinical symptoms of pancreatitis range widely from mild, self-limiting upper abdominal pain to multi-organ failure and sepsis with high mortality. Caerulein, a synthetic decapeptide originally extracted from the skin of the Australian amphibian Hyla cerulean, stimulates exocrine pancreatic secretion in a variety of mammals including humans.
Optional Endpoint
- PK/PD blood collections
- Cytokine/chemokine analysis via Luminex(R)
- Other sandwich ELISAs
- CBC/clinical chemistry analysis
- Soft tissue collection
- Histopathologic analysis
- Immunohistochemistry analysis
References:
- Wildi S, Kleeff J, Mayerle J, et al. Suppression of transforming growth factor β signaling aborts caerulein induced pancreatitis and eliminates restricted stimulation at high caerulein concentrations. Gut 2007;56:685-692.
- Lampel M, Kern HF. Acute Interstitial pancreatitis in the rat induced by excessive doses of a pancreatic secretagogue. Virchows Arch A Pathol Anat Histopathol 1977;373:97-117.
For more information about Non-Lethal Caerulein-Induced Pancreatitis (Rat, Mouse) contact us here.
Related Pages
General Inflammation
- Oxazolone Induced Ear Delayed Type Hypersensitivity (Mouse)
- mBSA Induced Footpad Delayed Type Hypersensitivity (Mouse)
- Carrageenan Induced Paw Edema (Rat & Mouse)
- Lipopolysaccharide Induced Cytokine Cascade (Rat, Mouse)
- IL-23 induced Psoriasis (Mouse)
- IMQ induced Psoriasis (Rat, Mouse)
- Monosodium Urate-Induced Gout
- Zymosan Induced Peritonitis
- Non-Lethal Cerulein-Induced Pancreatitis (Rat, Mouse)