Medial Meniscal Tear-Induced OA (MMT) in Rats

Overview:
Animal models of OA, including the rat medial meniscal tear (MMT) model, have been used fairly extensively for testing of potential anti-arthritic agents and disease modifying effects of treatments over the years.
Induction:
Animals are anesthetized with Isoflurane and the right knee area and lower leg are prepared for surgery. A skin incision is made from the distal patella to the proximal tibial plateau. The medial collateral ligament is transected just below its attachment to the meniscus, so that when the joint space opens, the meniscus is reflected toward the femur. The meniscus is cut at its narrowest point (away from the ossicles), and care is taken not to damage the tibial surface and to ensure the resulting transection yields a meniscus that is freely movable both anteriorly and posteriorly.
Disease Parameters/Progression:
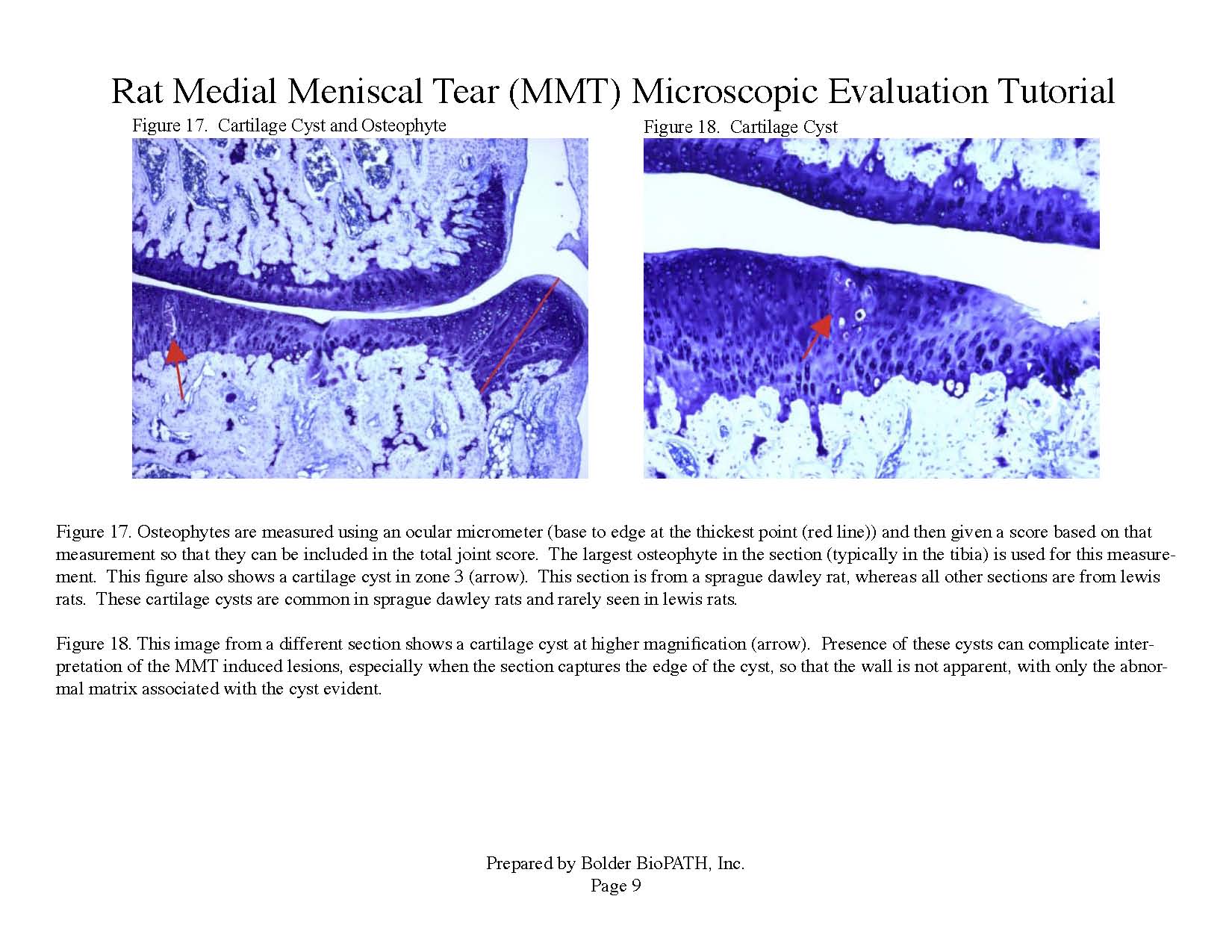
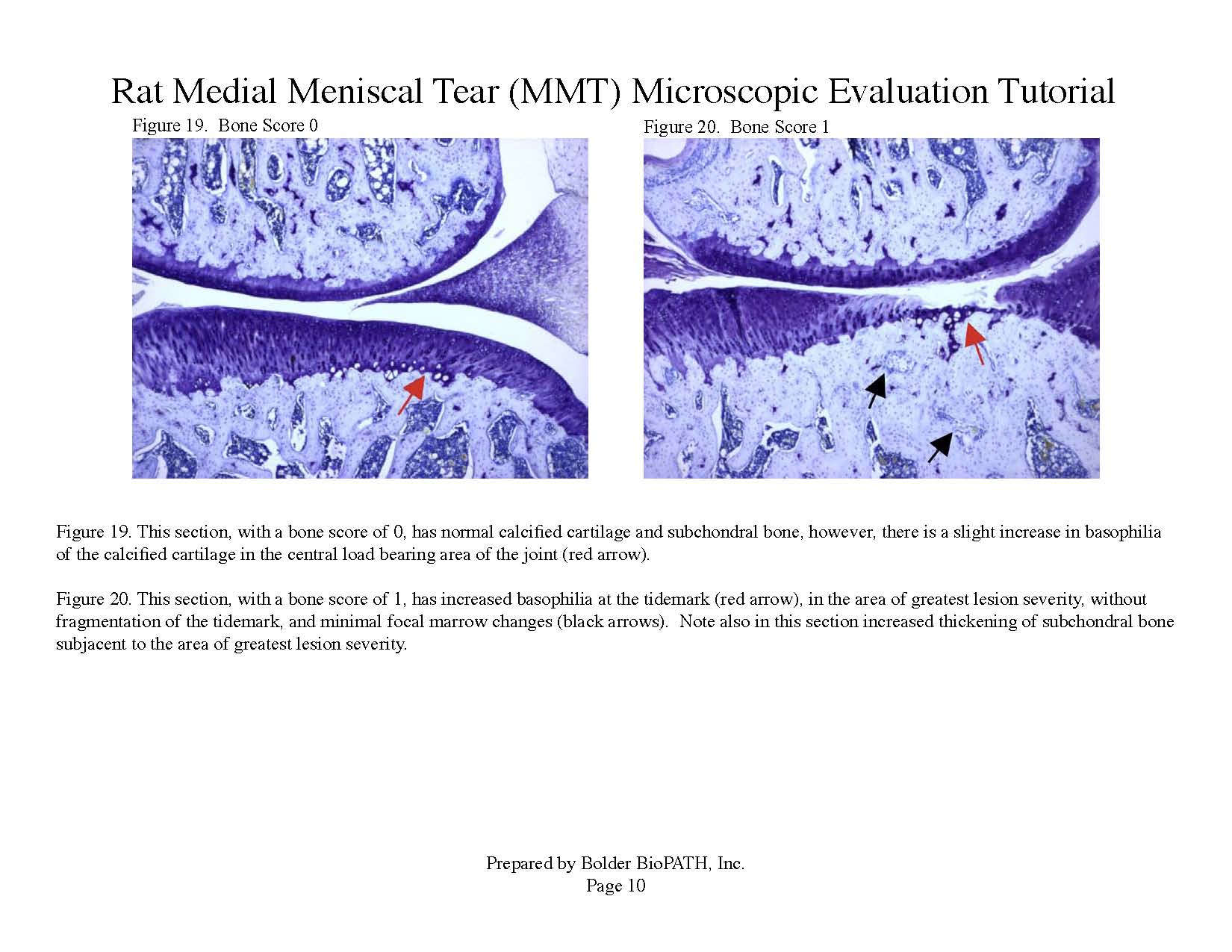
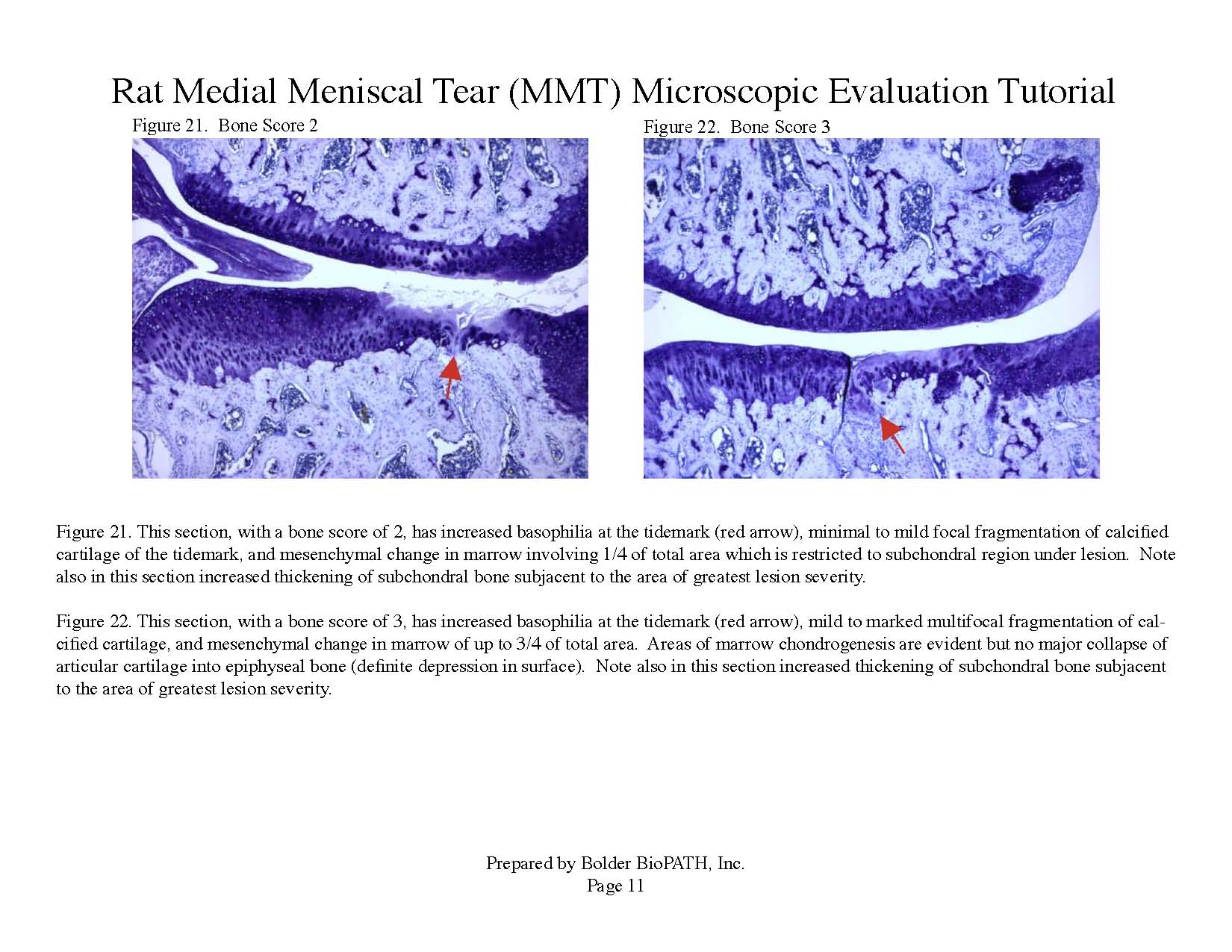
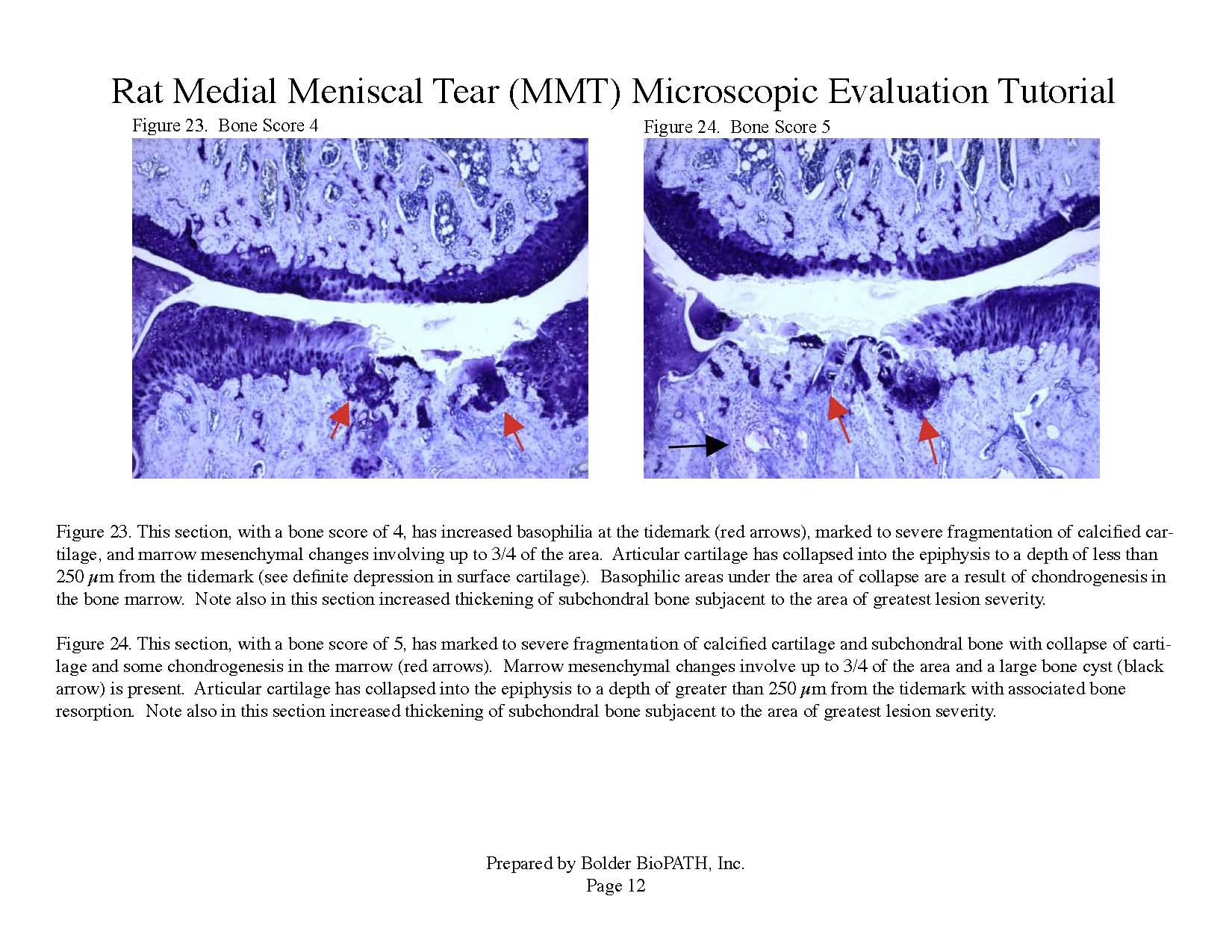
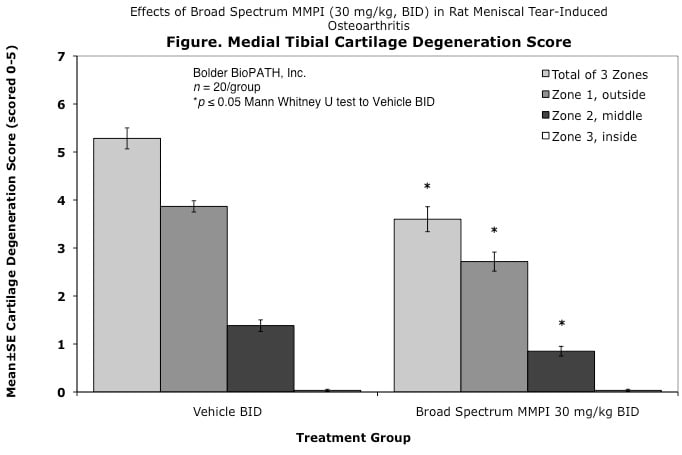
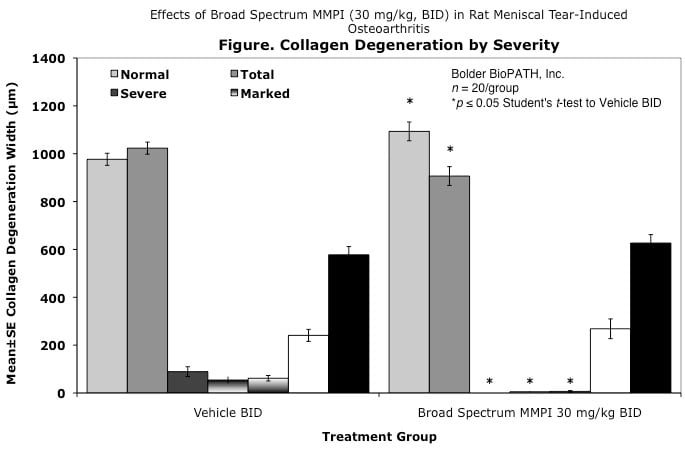
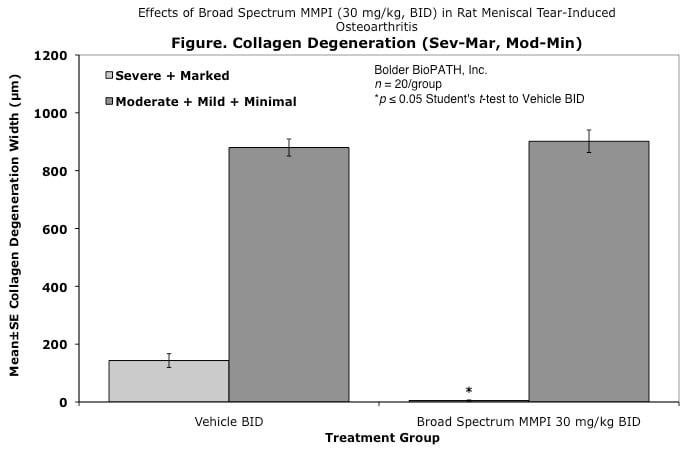
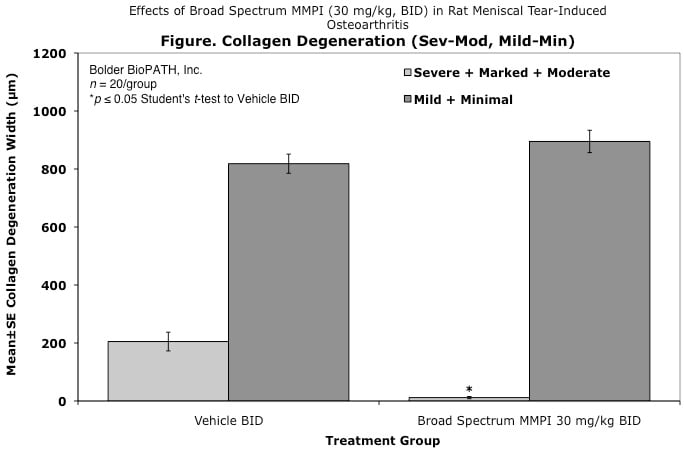
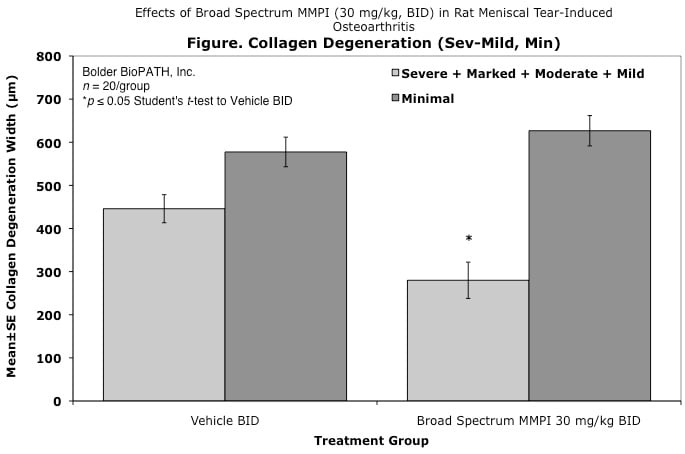
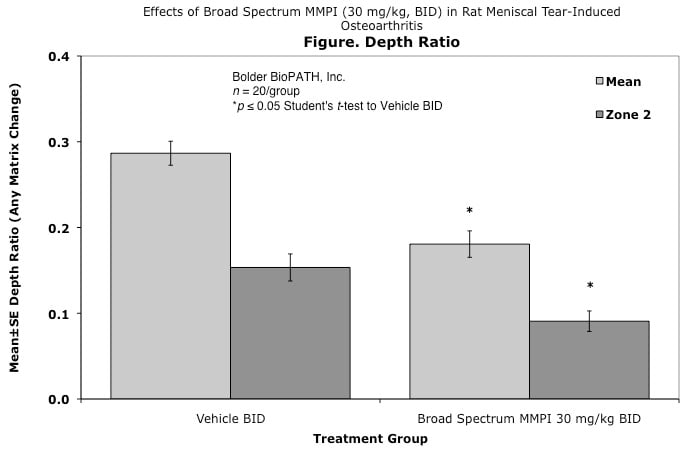
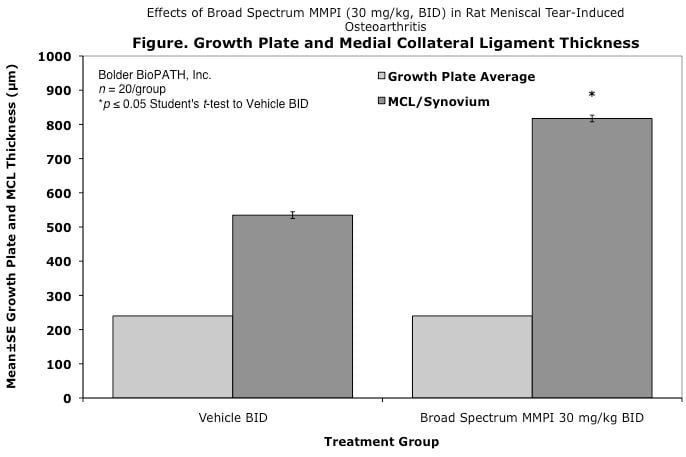
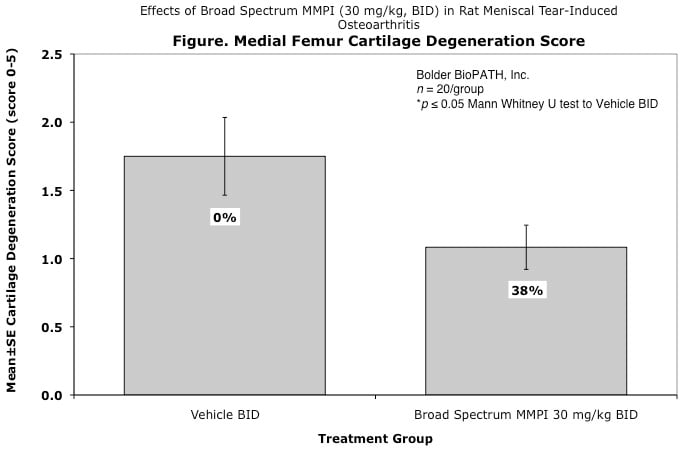
Cartilage degenerative changes develop progressively and, by 3 to 6 weeks post-surgery, tibial cartilage degeneration may be focally severe on the outer 1/3 of the tibia, with degenerative changes of lesser severity in the middle and inner 1/3. Osteophytes are ultimately quite large (medial tibia) and progressively increase in size. The model is progressive and results in total cartilage (to eburnated bone) in 12 months in virtually all rats. Evaluation of anti-degenerative therapies requires at least 1 to 3 weeks. A group size of 15 to 20 animals is generally sufficient to account for variabe lesion severity. Because cartilage degenerates rapidly in rats, this model constitutes an extremely high hurdle for the detection of protective effects. This is especially true for the outer one-third of the tibial cartilage, where collagen disruption and matrix loss are often quite severe. However, zonal analysis may result in detection of treatment effects in the middle and inner one-third of the tibia, areas in which mechanical trauma is not an important cause of pathogenesis. Substantial subchondral and epiphyseal bone changes occur in the medial tibia subjacent to the areas of greatest lesion severity. These changes range in magnitude and type from increased basophilia of the calcified cartilage with small fractures into subchondral bone to overt collapse of articular cartilage into areas of bone resorption in the epiphysis, surrounded by sclerosis of bone. This model therefore permits evaluation not only of chondroprotective effects, but also bone preserving activities.
Dosing Paradigms:
- Begin dosing X days prior to surgery or post surgery and continue until necropsy.
- Route of administration: SC, PO, IP, IV, IA
Clinical Assessment:
Animal body weights are measured weekly. Tactile allodynia and Gait analysis can be evaluated at multiple time-points.
Histopathological Assessment:
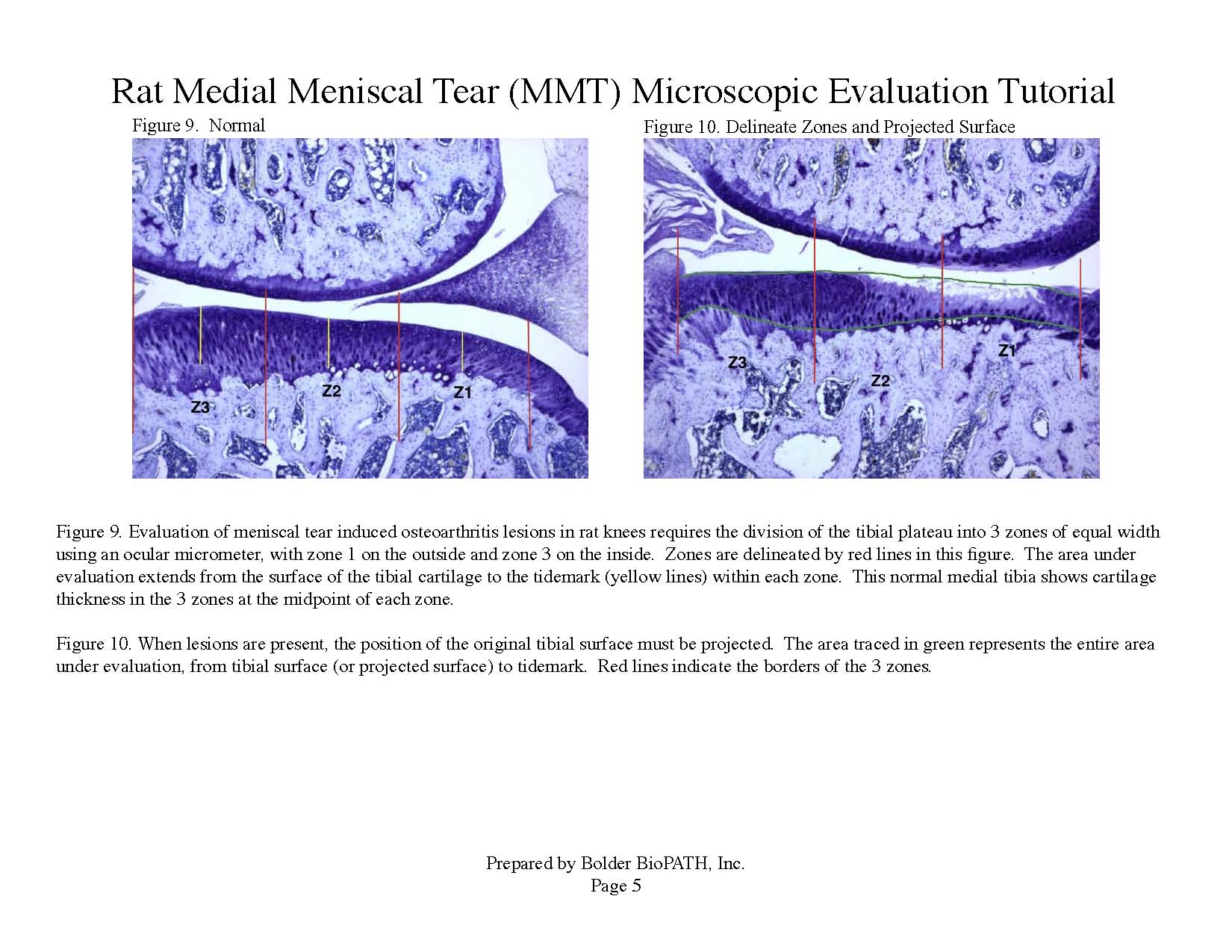
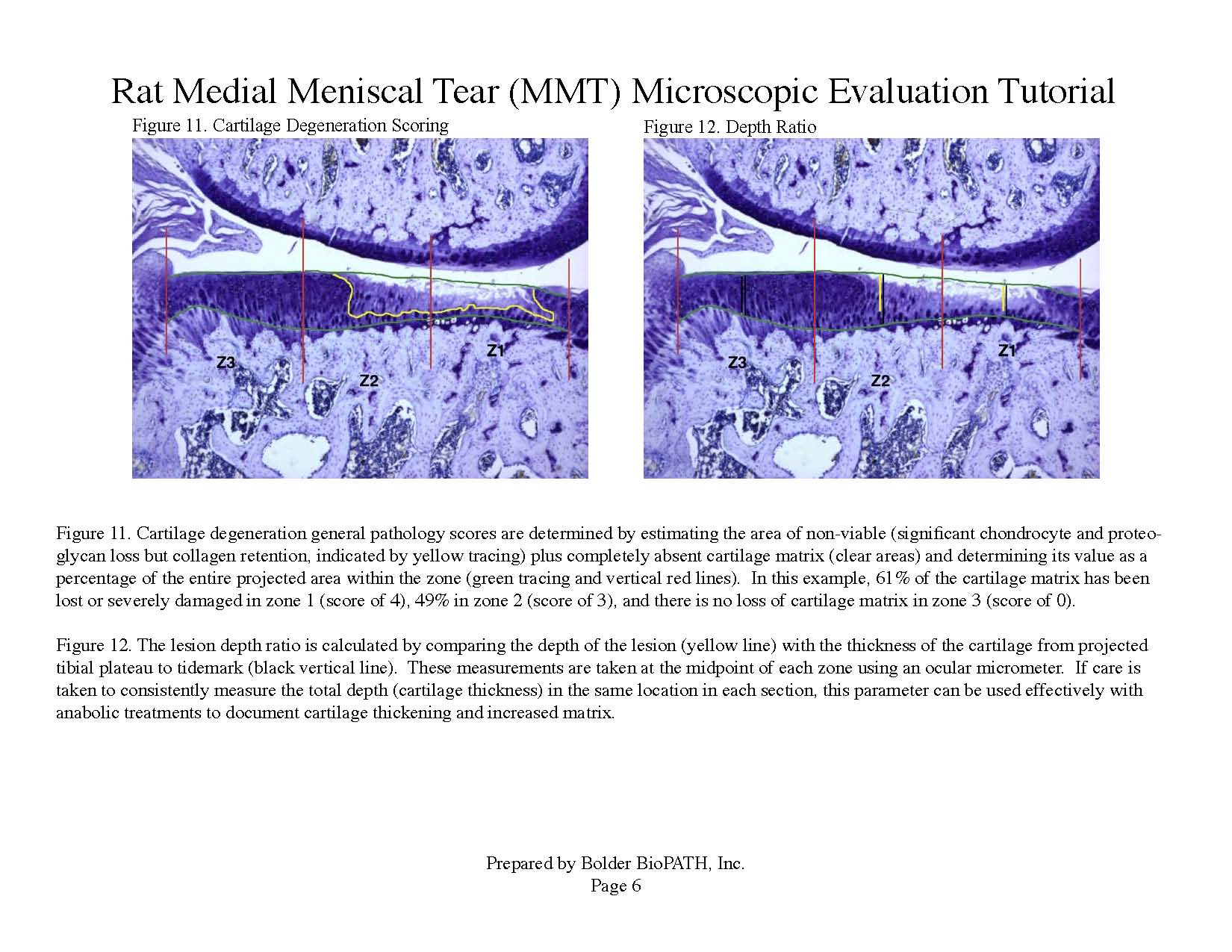
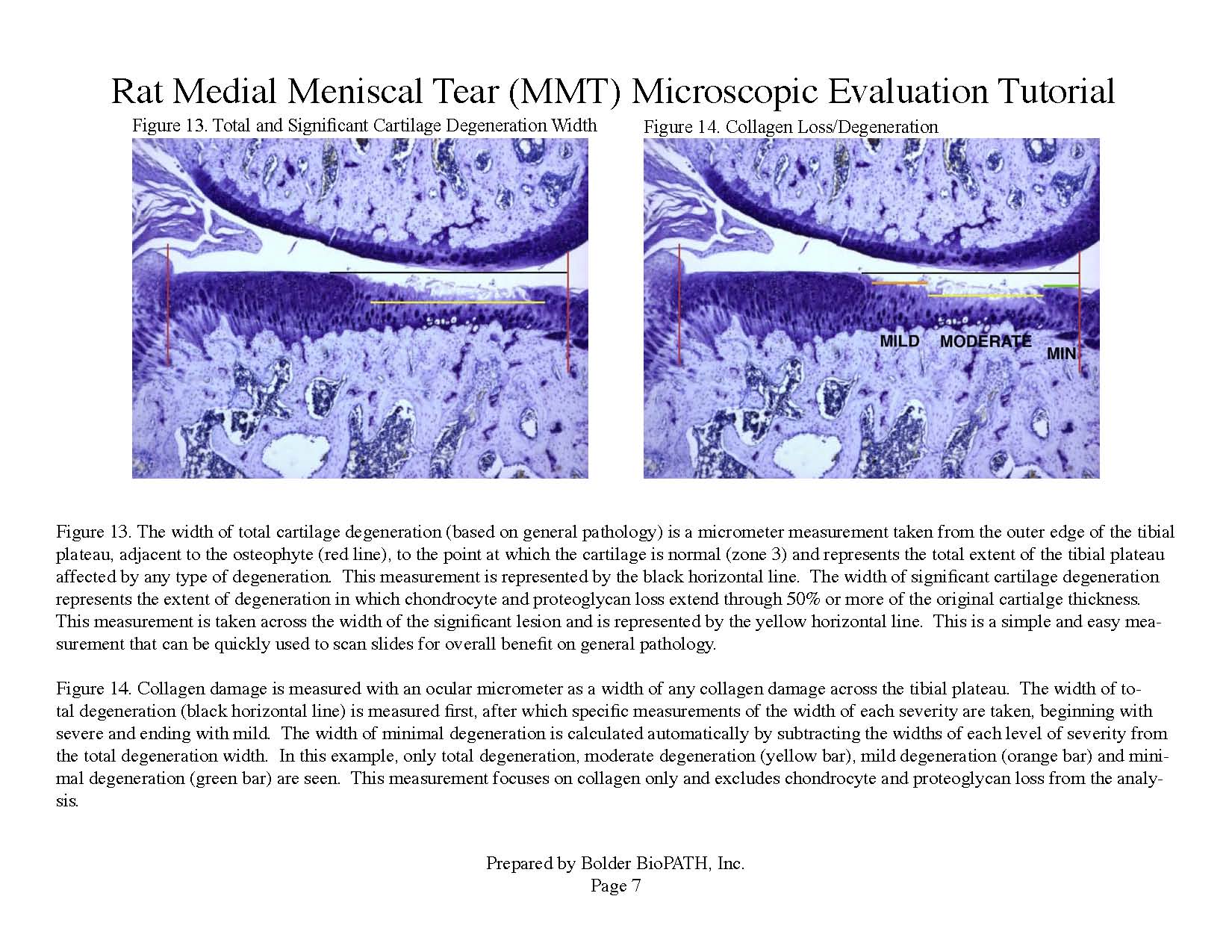
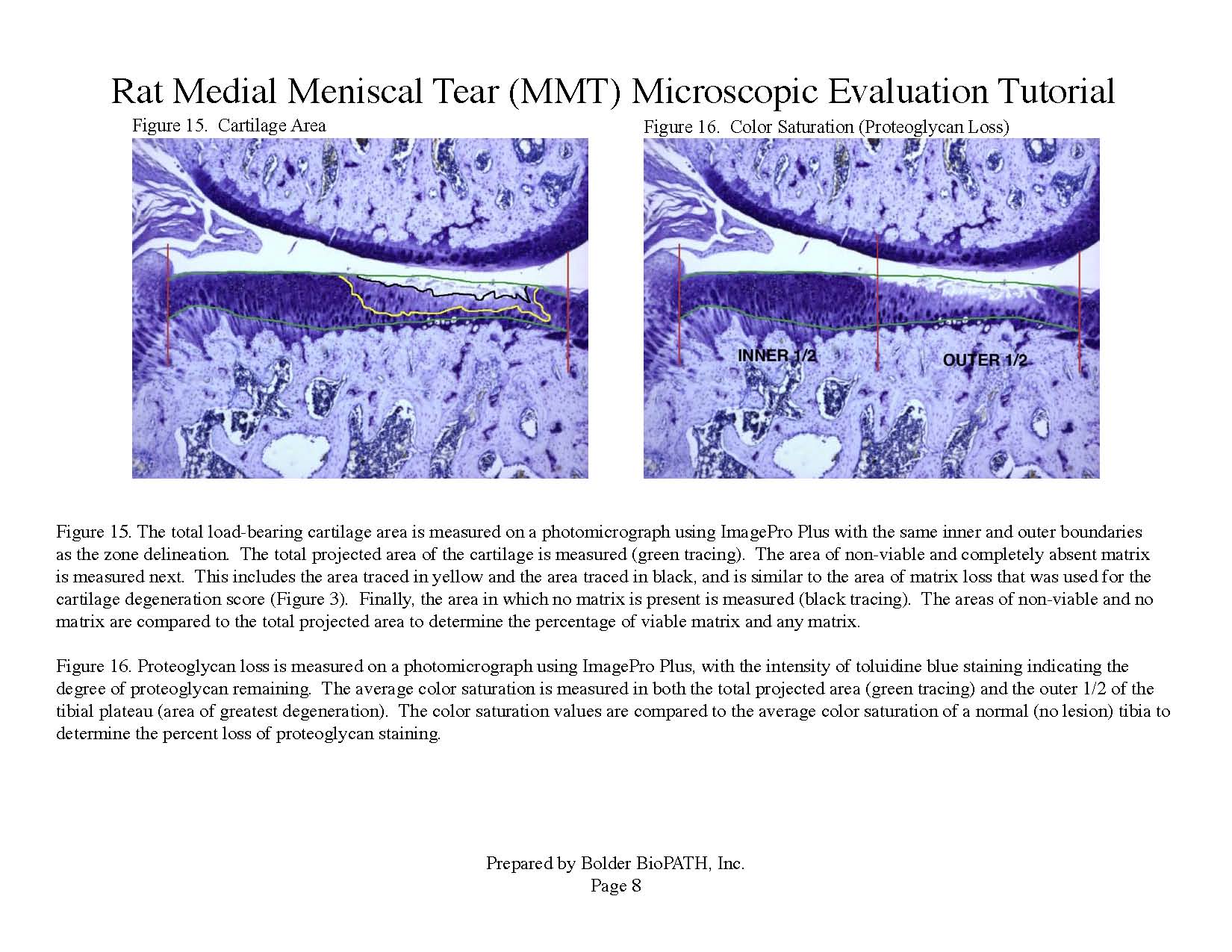
Operated joints are cut into two approximately equal halves in the frontal plane and embedded in paraffin. Three sections are cut from each knee at approximately 160 µm steps and stained with toluidine blue. Tissues are analyzed microscopically. The worst-case scenario for the two halves on each slide is determined and used for evaluation. The values for each parameter are then averaged across the three sections to determine overall values for each animal. Knees are examined microscopically by a board certified veterinary pathologist according to these methods.
Sample Data (Click on image to enlarge):
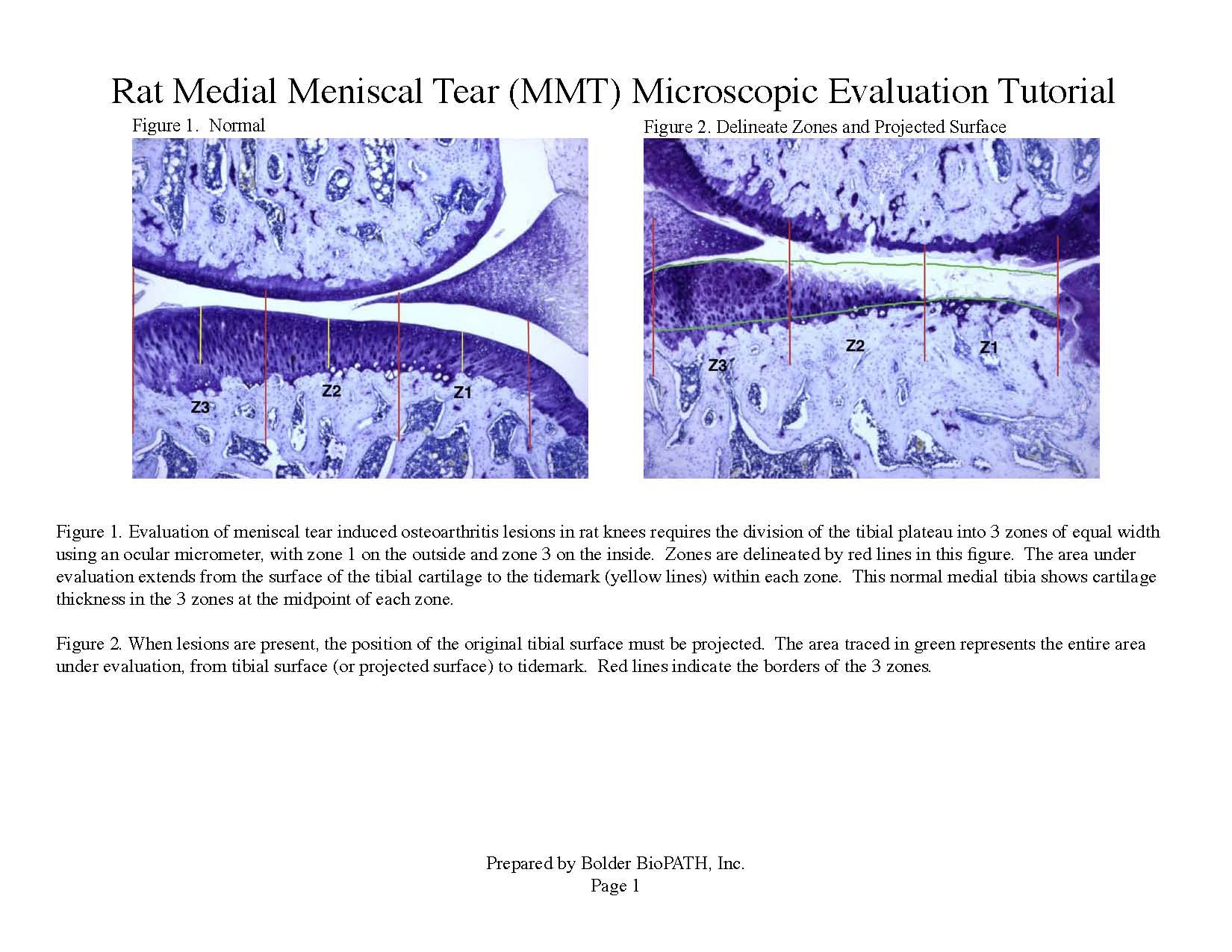
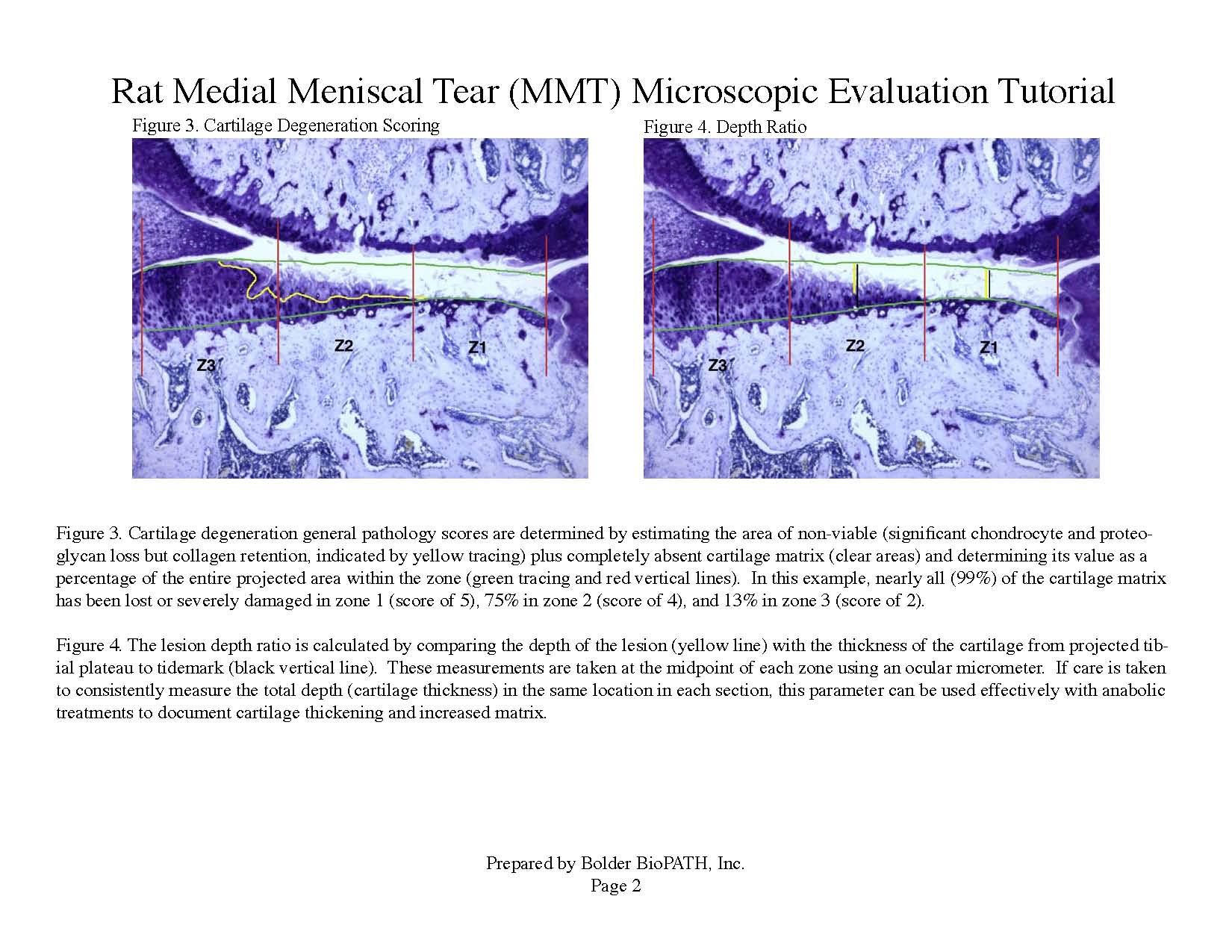
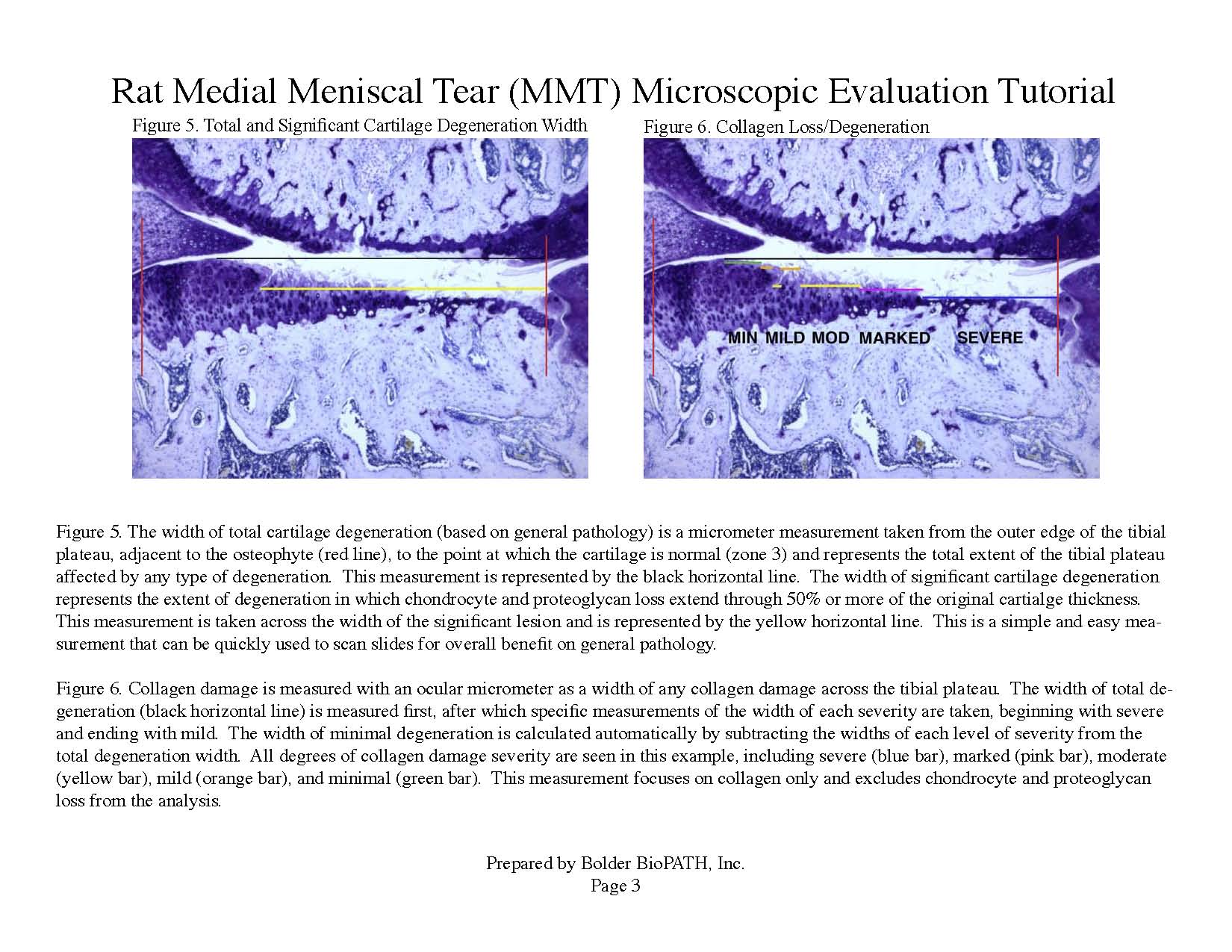
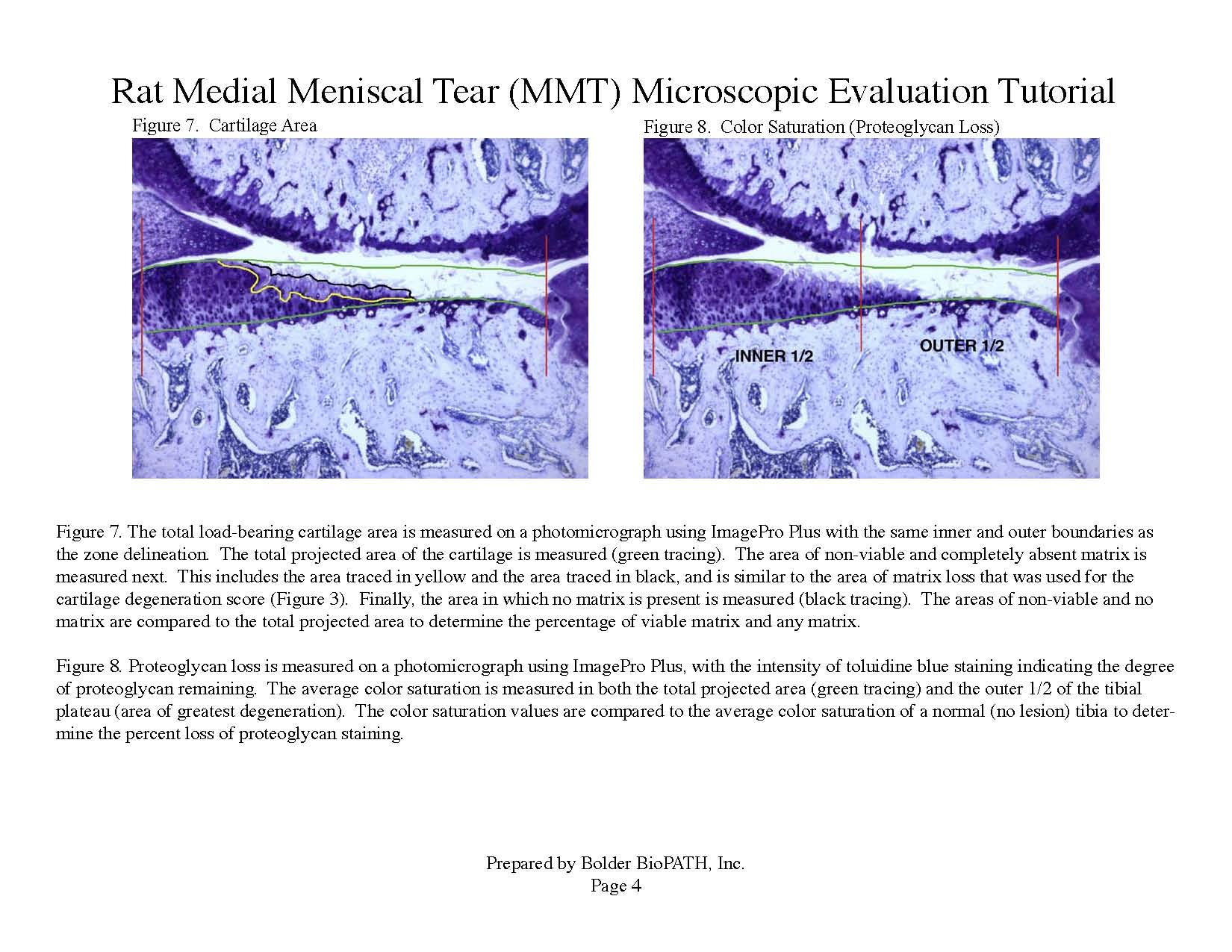
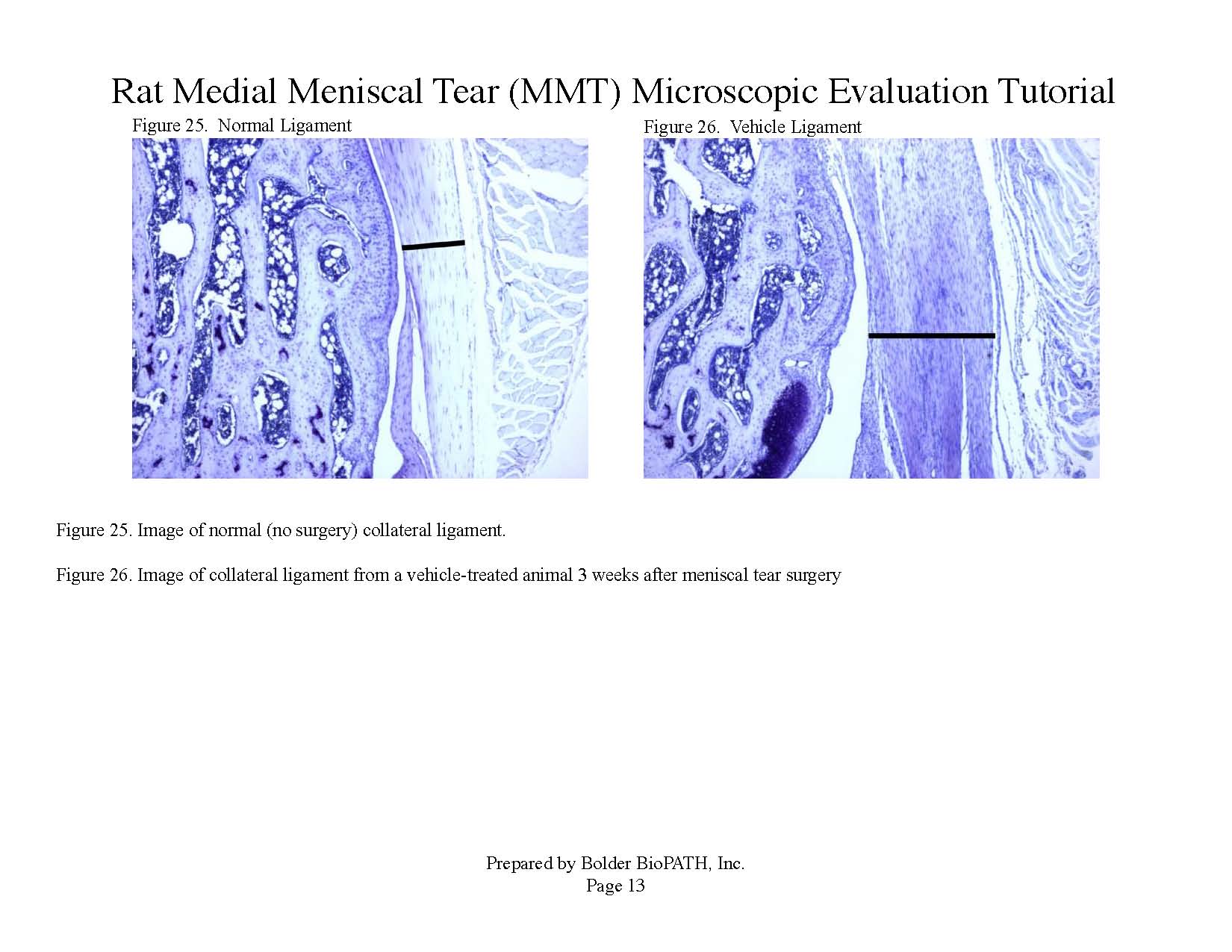
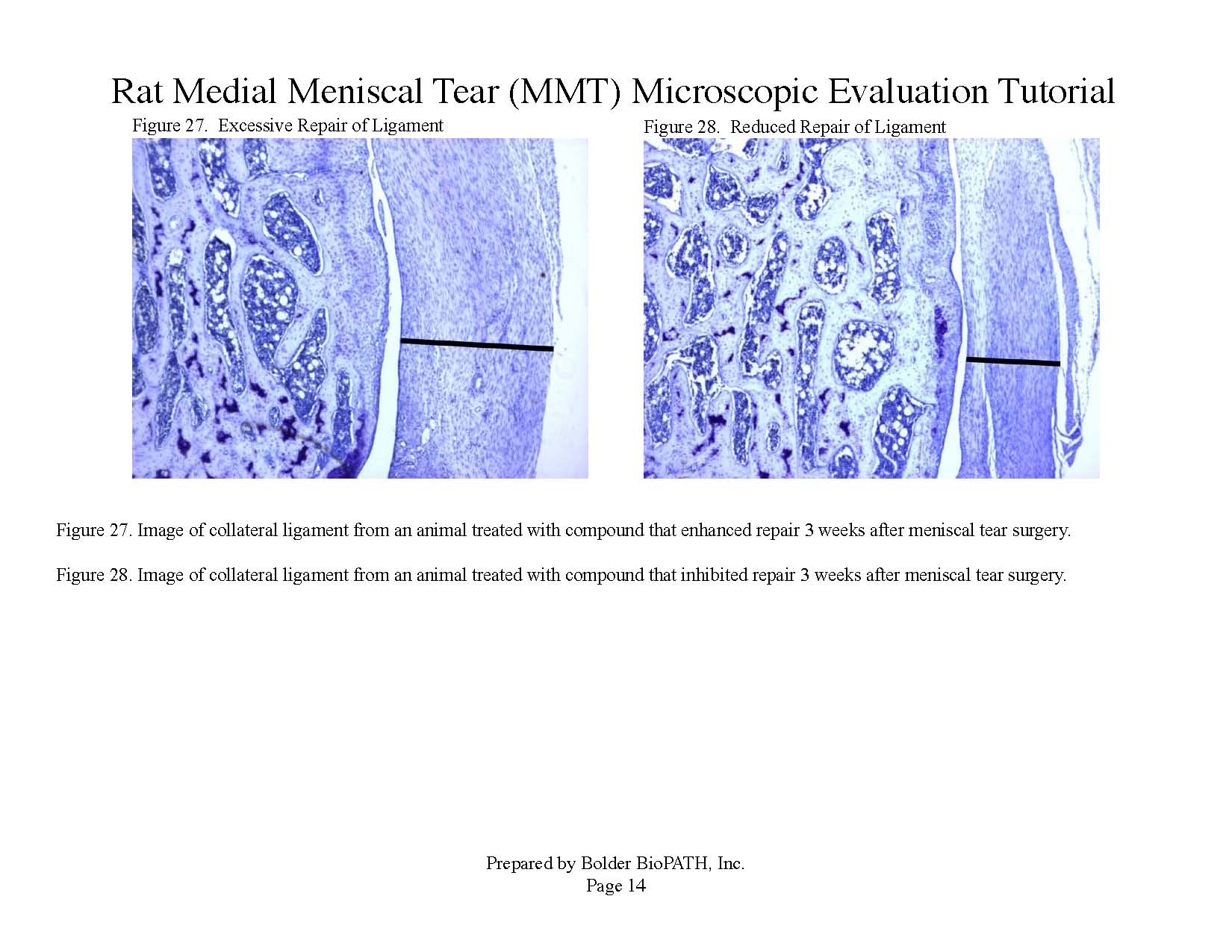
Photomicrographs: Rat Medial Meniscal Tear Microscopic Evaluation Tutorial
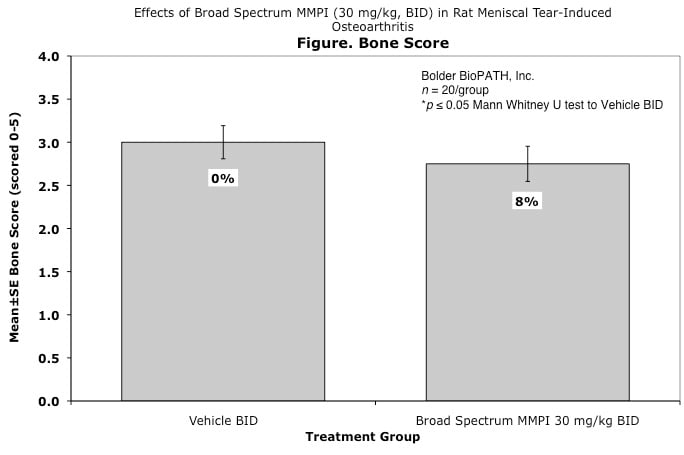
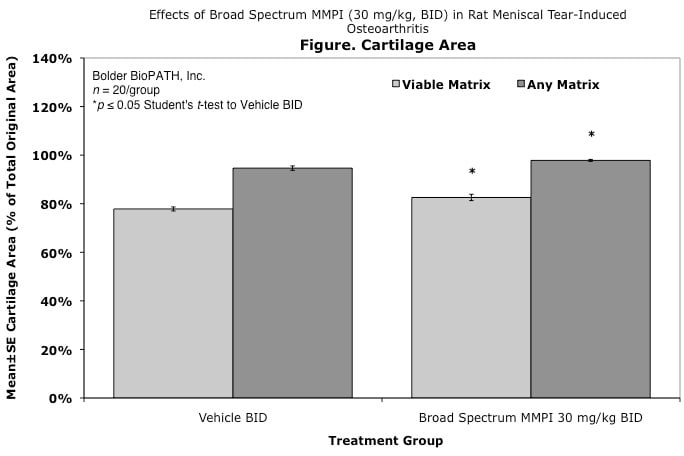
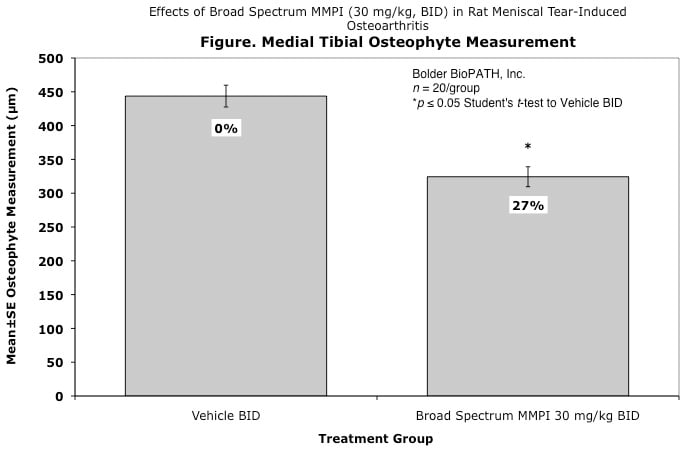
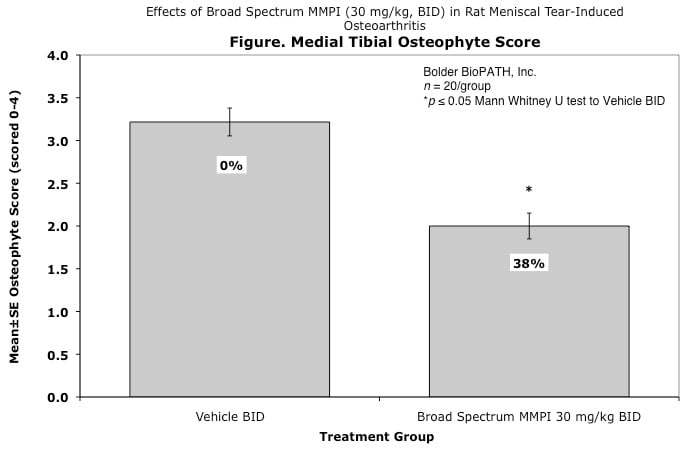
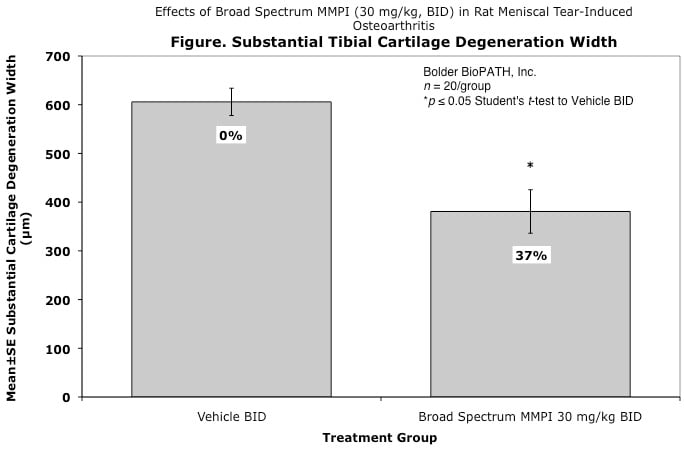
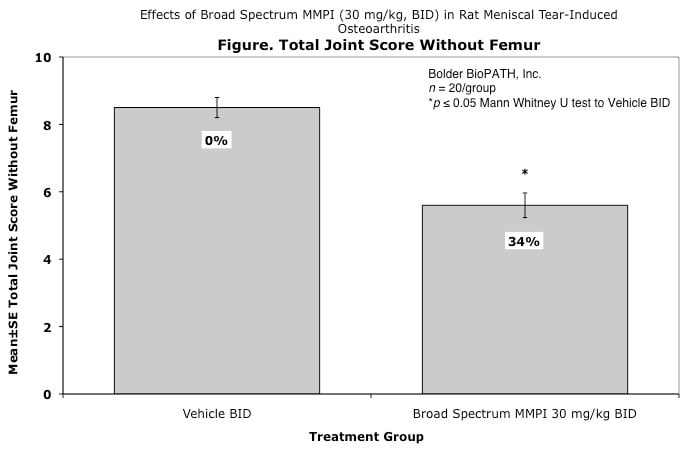
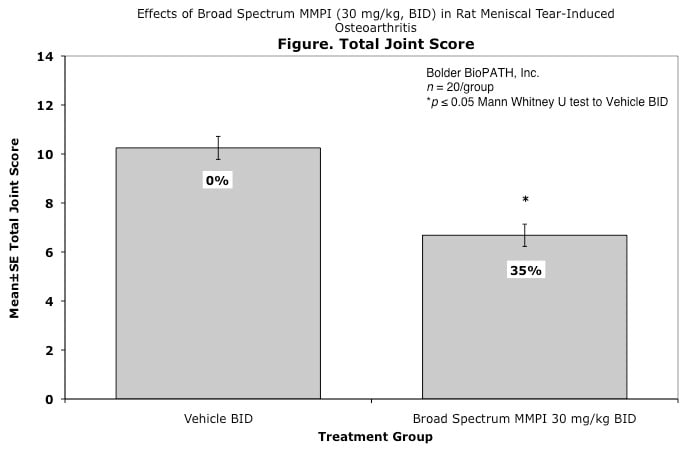
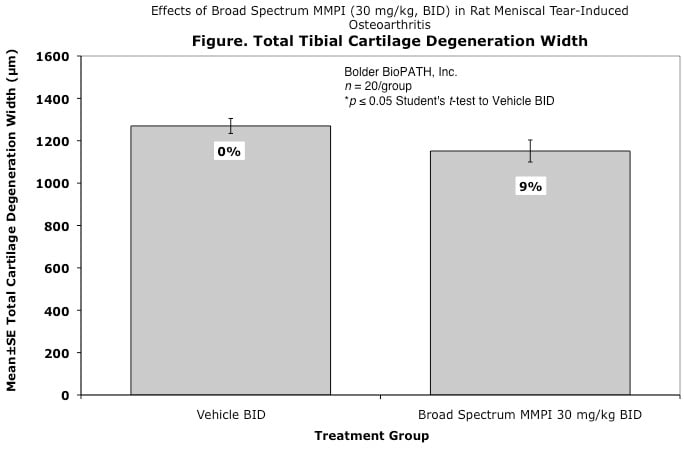
Effects of Broad Spectrum MMPI (30 mg/kg, BID) in Rat Meniscal Tear-Induced Osteoarthritis
Notes:
One advantage of using rats is that they are commonly used in toxicology testing. Efficacy in this species in combination with toxicology evaluation allows for the generation of a therapeutic index for compounds under evaluation. Results can be obtained in relatively short periods and the response of the animals to surgery is very consistent. Inhibitors of MMP-13 (collagenase) are consistently active in the rat model. This model has also been used to evaluate cartilage repair strategies. Repeated injections of FGF-18 into rats 3 weeks after the OA lesions were established led to chondrogenesis and the filling of defects in areas of severe degeneration (Moore, 2005).
Optional Endpoint
- Gait analysis
- PK/PD blood collections
- Cytokine/chemokine analysis via Luminex(R)
- Other sandwich ELISAs
- CBC/clinical chemistry analysis
- Soft tissue collection
- Histopathologic analysis
- Immunohistochemistry analysis
References:
- Janusz MJ, Bendele AM, Brown KK, Taiwo YO, Hsieh L, Heitmeyer SA, Induction of osteoarthritis in the rat by surgical tear of the meniscus: Inhibition of joint damage by a matrix metalloproteinase inhibitor. Osteoarthritis Cartilage. 2002 Oct;10
- Gerwin N, Bendele AM, Glasson S, Carlson CS. The OARSI histopathology initiative – recommendations for histological assessments of osteoarthritis in the rat. Osteoarthritis Cartilage. 2010 Oct;18
- Moore EE1, Bendele AM, Thompson DL, Littau A, Waggie KS, Reardon B, Ellsworth JL. Fibroblast growth factor-18 stimulates chondrogenesis and cartilage repair in a rat model of injury-induced osteoarthritis.
Osteoarthritis Cartilage. 2005 Jul;13(7):623-31.
Related Pages
- Partial Medial Meniscectomy-Induced Arthritis in Canine
- ACL Transection-Induced Arthritis in Canine
- Medial Meniscal Tear-Induced OA (MMT) in Rats
- Monoiodoacetate-Induced Arthritis (MIA) in Rats
- Destabilization Of The Medial Meniscus (DMM) in Rats & Mice
- Partial Lateral Meniscectomy Induced OA in Rabbits
- Spontaneous Osteoarthritis in Guinea Pigs
- Meniscal Tear-Induced Arthritis in Guinea Pigs